What Are the Most Common Urological Conditions Men Face?
The prostate is a small gland that helps make semen. It’s found just below the bladder. It allows urine to evacuate and which surrounds the urethral canal, is often implicated in urinary disorders linked to prostate diseases due to its anatomical location.
Located between the anus and the genitals, the perineum stabilizes the pelvis and supports all of the organs of the abdomen. Made up of muscles and ligaments, it ensures the proper functioning of the sphincters which allow the anus and urethra to open and close.

Some Anatomical Reminders to Better Understand
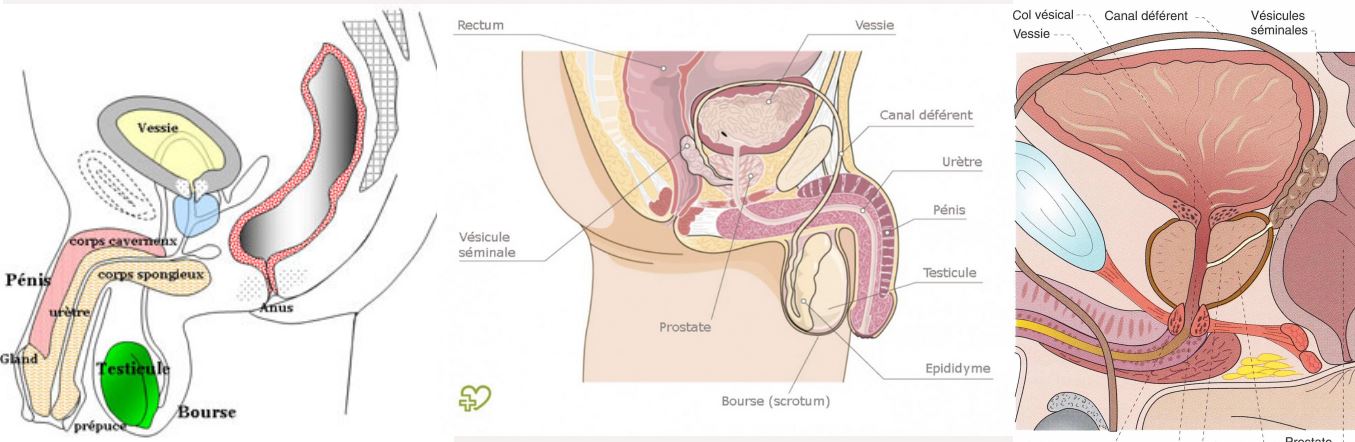
In males, the perineum lies just below the pelvic floor muscles, which support the bladder and bowel. The perineum protects the pelvic floor muscles and the blood vessels that supply the genitals and urinary tract. The perineum also protects the nerves used to urinate or have an erection. The pudendal nerve runs through the perineum and branches out into various parts of genitals, pelvic floor muscles and anus. This complex nerve network makes the male perineum sensitive to sexual sensations.

Common Bladder Problems in Men
- Urinary disorders include all clinical signs that impact urination. This may include daytime urinary frequency (abnormally frequent urge to urinate more than 7 times a day), nocturia (getting up more than twice at night), dysuria (difficulty urinating), burning when urinating, or even urine retention.
- Benign prostatic hyperplasia, also called benign prostatic hypertrophy (BPH) is a condition in men which the prostate is enlarged. It is a health issue that becomes more common with age. An enlarged prostate can cause blocking the flow of urine out of the bladder, bladder urinary tract or kidney problems.
- Prostate cancer is one of the most common male cancers. He provokes urinary disorders, especially when the disease has progressed to an advanced stage. Prostate cancer can in fact be asymptomatic at an early stage.
- Prostatitis or chronic pelvic pain syndrome causes various urinary disorders and can be induced by a treated bacterial infection. Most often there is inflammation of the prostate, which in some patients becomes chronic.
- Other causes can explain urinary symptoms. These are particularly the case of urinary infection. Men are less affected due to the anatomy of the male urogenital system which provides natural protection against bacterial infections. However, urinary infection can manifest itself in the urethra (urethritis), the prostate (prostatitis), the kidneys (pyelonephritis) and more rarely in the bladder (cystitis).
- In older men, the bacterial infection is mainly localized on the prostate, leading to an enlargement, difficulty urinating and fever. The bacteria involved is usually Escherichia coli.
- Neurological control of the bladder occurs at the level of the central nervous system and the spinal cord. Many neurological diseases cause bladder and sphincter disorders, which can impact bladder emptying and/or filling: multiple sclerosis, Parkinson’s disease, stroke, spinal cord paralysis, etc. Affected patients have an increased risk of manifesting incontinence. urinary tract, urinary retention or other urological problems. These disorders belong to a specialty: neuro-urology.
- Bladder cancer. The less common types of bladder cancer such as squamous cell carcinoma, adenocarcinoma, and small cell carcinoma have a greater tendency to be muscle invasive compared to urothelial carcinoma.
- Benign bladder tumor. The majority of bladder tumors are non-cancerous. Of several types, they cause different bladder problems in men.
- Kidney stones (also called renal calculi, nephrolithiasis or urolithiasis) are hard deposits made of minerals and salts that form inside your kidneys. Diet, excess body weight, some medical conditions, are among the many causes of kidney stones.
- Kidney cancer. It often causes no symptoms and is therefore discovered by ultrasonograpy or biological tests. It can appear as blood in the urine. This is especially true since the bleeding in this case is often intermittent and completely painless.
Other Causes in Young Male
- Urethritis (urinary tract infection due to a sexually transmitted infection).
- Benign prostatic hypertrophy (rare, but not impossible).
- Burning urination, is frequently caused by urethritis and prostate problems as well as sexual transmitted infections, genital herpes and personal care products that irritate.
- Post-micturition dribble (PMD) is the involuntary loss of urine immediately after urination. It is a post-micturition symptom and is more common in males, with can several causes, but one of the most common in younger men is a narrowing of the bladder neck, or hypertonia.
- Overflow incontinence. Is a frequent or constant dribbling of urine due to a bladder that doesn’t empty completely.
- Cycling predisposes to various disorders, localized to the level of the perineal area. T his sport, practised while seated, places enormous demands on the muscles of the perineum. These are mainly observed within the framework of intensive practice.

Les techniques utilisées dans le traitement de l’adénome de prostate
Diagnosis and Evaluation
- Examination of the prostate by inserting a gloved finger into your bottom – called digital rectal examination Urinalysis is a test of your urine used to detect and manage a wide range of disorders, such as urinary tract infections, kidney disease and diabetes.
- Urinary cytology is most helpful in diagnosing invasive high-grade (the cancer cells grow and spread quickly) tumors and carcinoma in situ.
- Bladder Tumor Antigen, or BTA. STA and TRAK are found in bladder cancer cell lines and inhibit the complement cascade to prevent cell lysis.
- Prostate specific antigen, or PSA, must be below 2.5 ng/ml before age 50 and less than 6.5 ng/ml before the age of 80. It is increased in prostate cancer but also in other common prostate pathologies.
- The Gleason score is of great value. Cancers with a higher Gleason score are considered more aggressive and their prognosis is worse. Scores are between 2 and 10.
- Bladder ultrasound allows you to examine its wall and look for the presence of a polyp, of a stone or abnormal thickening. It allows you to check if the bladder is emptying well.
- Prostate ultrasound is minimally invasive and allows information such as: the size of the prostate, the presence of a nodule, the obstructive nature and bladder emptying.
- Urethrocystoscopy using a camera and under local anesthesia explores the sector urological (urethra, prostate, bladder), in order to detect an anomaly. Prostate biopsy involves taking tissue samples from the prostate.
- Prostate for laboratory analysis to confirm benign or malignant character.
- Urodynamic tests focus on how well your bladder can hold and empty urine. Urodynamic tests can also show whether your bladder is contracting when it’s not supposed to, causing urine to leak.
What are the treatment options for prostate diseases
- Among heat-based modalities, more therapeutical options are viable, i.e., radiofrequency ablation (RFA), microwave ablation (MWA), and high-intensity focused ultrasound (HIFU).
- Innovative treatment for BPH : The UroLift™ System The UroLift® implant has been developed as a mechanical means of widening the prostatic urethra and providing relief from lower urinary tract symptoms through a minimally invasive procedure. performed as a same-day outpatient, including the office setting, under local anesthesia. This mechanical approach avoids extensive post operative retention, irritation, and infection.
- Innovative Treatment for BPH: Rezūm Water Vapor Therapy Is a non-surgical treatment that uses the natural energy stored in water vapor, or steam, to remove excess prostate tissue that is pressing on the urethra. When the steam contacts the prostate tissue, all the stored energy is released into the tissue. There are no incisions, and typically it does not require general anesthesia. It has also been shown to preserve sexual function.
- Innovative treatment for prosate cancer: Prostatic artery embolization (PAE) PAE proves beneficial in men who have prostate cancer by combining optimal LUTS improvement with maximal prostate volume reduction prior to radiation therapy. It has a high rate of success, with over 90% of men experiencing relief in the first year. Unlike other treatments that may have unwanted sexual side effects, PAE does not affect sexual performance. PAE is generally a well-tolerated with only minor symptoms.
- Innovative Treatment for Enlarged Prostate: Laser enucleation A laser is used to cut and remove the excess prostate tissue that is blocking the urethra. Minimally invasive HoLEP procedure, considered the gold-standard surgery for enlarged prostate, is enabling this patient to resume a normal lifestyle. The main advantage of HoLEP over some other methods is the large volume of prostate tissue that can be safely removed.
What are the treatment options for prostate cancer
- Watchful waiting Watchful waiting is often recommended for older men when it’s unlikely the cancer will affect their natural lifespan.
- Non surgical options :
- Radiotherapy nvolves using radiation to kill cancerous cells. This treatment is an option for curing prostate cancer that has not spread beyond the prostate or has not spread very far.
- Hormone therapy is often used in combination with radiotherapy. Patient may receive hormone therapy before undergoing radiotherapy to increase the chance of successful treatment.
- Trans-urethral resection of the prostate (TURP) TURP is a procedure that can help relieve pressure from the tube that carries urine from your bladder out of your penis to treat any problematic symptoms the patient may have with urination.
- Cryotherapy It is a method of killing cancer cells by freezing them. It’s sometimes used to treat localised prostate cancer that has not spread beyond the prostate gland.
- Chemotherapy This therapy destroys cancer cells by interfering with the way they multiply. It does not cure prostate cancer but can keep it under control to help you live longer.
- Surgical options : Surgery is a common choice to try to cure prostate cancer if it is not thought to have spread outside the prostate gland.
- Radical (Open) Prostatectomy The surgeon creates an incision in one of two possible areas in the lower abdomen, extending from the belly button to the pubic bone. He removes the prostate and nearby tissues. A radical perineal prostatectomy is performed through an incision made between the anus and the scrotum.
- Laparoscopic Radical Prostatectomy Laparoscopic approaches involve using smaller incisions and long surgical tools to take out the prostate. The surgeon uses an instrument with a video camera on the end to look inside the patient’s body. This method usually results in less pain and blood loss, faster recovery times and shorter hospital stays.
- A robot-assisted laparoscopic radical prostatectomy is performed with the aid of a robot controlled by a surgeon. Multiple small incisions are made in the abdomen to allow for the movement of the robotic arms and camera. This robotic approach (Da Vinci ) may improve the surgeon’s precision and maneuverability.
What Could Happen After A Prostatectomy ?
Simple prostatectomy provides long-term relief of urinary symptoms due to an enlarged prostate. Although it’s the most invasive procedure to treat an enlarged prostate, serious complications are rare. Most men who have the procedure generally don’t need any follow-up treatment for their BPH.
In addition to the risks associated with any surgery, risks with radical prostatectomy include:
Bladder Problems
Incontinence after prostate treatment (IPT) is a known complication of prostate treatment that can significantly adversely impact quality of life. IPT is the main result of urethral sphincter deficiency or detrusor overactivity. The symptoms could be : leakage of urine when sneezing or laughing, or feel an urgent need to go to the bathroom. IPT can greatly improve in the first one to two years with conservative therapies. Though minor incontinence still occurs with robotic surgery, most men will have full control of their bladder after about six to eight weeks.
Changes in Sex Life
Nearly all men will experience some erectile dysfunction (ED) for the first few months after prostate cancer treatment. Most men experience some ED after their prostate is removed, but it can take six months or even up to a year for the affected nerves to recover from surgery. Another change to expect in sex life is that, because the seminal vesicles are removed during surgery, you won’t ejaculate semen during orgasm.
Management of Urinary Incontinence Following Prostatectomy
Treatment of overactive bladder
Conservative treatments are offered: lifestyle modifications, behavioral therapy, pelvic floor muscles exercices.
Biofeedback therapy, electrical stimulation, extracorporeal magnetic stimulation.
Pharmacotherapy with anticholinergic agents.
If this fails, other therapeutic options may be offered to the patient, such as:
Transcutaneous neurostimulation of the posterior tibial nerve.
Injection of botulinum toxin A into the bladder (Botox®).
Sacral neurostimulation (SNS).
Treatment of stress urinary incontinence
Conservative treatments are offered: Kegel exercises (KE) are the most popular and used among the pelvic floor muscles exercices. Electrical stimulation sessions with probes or extracorporeal magnetic stimulation are also offered. Duloxetine works by stimulating the pudendal nerve, thereby increasing tension in the urethral sphincter and relaxing the detrusor muscle.
In the event of failure and depending on the severity of the incontinence, other solutions are:
Bulking agents may be an attractive alternative. Male slings aim to reposition the bulbar urethra, moving it to a proximal position.
Regarding invasive management of this type of urinary incontinence, the AMS 800 remains the first choice for moderate-to-severe forms.
Many men are afraid of IPT, and sometimes may decide to not undergo surgery. The identification of the key factors (age, race, height and weight, lifestyle) that predict presentation of UI and recovery of urinary control after RP could be a very useful tool.
The conservative treatments remain the first-line therapy, with PFME as the best choice for its easy accessibility and the shortened recovery time. Among the pharmacologic treatments, duloxetine is still an off-label drug, offered only for a temporary improvement of symptoms.
The pelvic muscle floor training (PMFT) is the first treatment to offer to patients with UI after RP. Various studies observed significant differences among the PMFE regimen adopted: number and duration of contractions, session frequency per day, and the presence or absence of therapist. A specific procedure for PFME after radical prostatectomy is needed because this would reduce the heterogeneity of the data.
Male slings emerged as a non-inferior minimally invasive alternative treatment to artificial urethral sphincter. Slings aim to reposition the bulbar urethra, moving it to a proximal position.
Regarding invasive management of IPP the artificial urethral sphincter remains the choice for severe forms.
There are different treatment options
Oral medications relax the muscles in the penis, allowing blood to rapidly flow in. On average, the drug take about an hour to begin working, and the erection-helping effects can last from 8 to 36 hours. About 75% of men who undergo nerve-sparing prostatectomy or more precise forms of radiation therapy have reported successfully achieving erections after using these drugs.
Physiotherapy including PFME and electrical stimulation with a specific focus on electrical magnetic stimulation.
The vacuum constriction device creates an erection mechanically by forcing blood into the penis using a vacuum seal. A rubber ring rolled onto the base of the penis prevents blood from escaping once the seal is broken.
Invasive treatments include implants or vascular surgery. The range of conditions we manage include Penile prosthesis complications, penile vascular abnormalities, penile curvature, and abnormally prolonged erection consequences.
Psychological treatment is an important adjunct to managing erectile dysfunction.

